In any war, the survival and health of serving personnel are largely due to the efforts and organisation of their medical personnel. The Australian doctors, dentists, nurses, stretcher-bearers and orderlies who served in Korea were no exception: they faced a wide variety of medical problems and challenges over the course of the war. Some Australian doctors who served in Korea were young, and had received little or no specific medical training for the trauma and injuries they would face there.
Apart from battle-related wounds, weather was a major factor in poor health, particularly among the ground troops who were forced to live in the cold of winter and in the extreme heat of summer. During the first year of the war, casualties were caused roughly in equal numbers by enemy action and the cold.
The incidence of frostbite was so severe in the first winter of 1950-51 that many of those afflicted had to be evacuated to Japan for treatment, which sometimes included amputation.
Medicines, including penicillin, froze and medical personnel expecting casualties warmed phials of medication in their pockets. In summer, heat and poor sanitation caused their own medical problems.
The maintenance of good hygiene was crucial.
Living in trenches was also responsible for medical complications, just as it had been for soldiers on the Western Front in the First World War. A condition called "Trench Foot" in the First World War and "Rice-Paddy Feet" in Korea was the same problem.
As in most wars, new techniques in medicine were pioneered. Australian medical teams in Korea developed new treatments in the repair of damaged blood vessels, saving many damaged limbs from amputation.
Moving casualties out
Because of medical evacuations by helicopter, the time taken to transport wounded to an established and well-supplied medical facility was normally quite short. However, this method had its limitations. Only two stretcher cases and two walking wounded soldiers could be evacuated at a time, and they could not receive treatment while in transit. In snowy conditions, when helicopters could not be used, medical evacuations had to be undertaken on the ground, often taking many hours to transport wounded to Regimental Aid Posts (RAP).
In the face of the rough terrain and the poor condition of local roads, helicopter evacuation was frequently the only option.
Aerial evacuation also decreased the need for medical teams to be near the front-lines, or to be at risk of being captured as prisoners, a risk for many medical personnel during the Second World War. Nonetheless, at the front lines there were still stretcher bearers and medical personnel working in the battalions or as part of a field ambulance, who recovered the wounded and applied first aid.
Nurses
Twenty nurses of the RAAF served in Korea, assisting with the evacuation and care of the wounded. In Japan, there was a large general hospital based in Kure, which received many casualties that were evacuated by air. In Iwakuni, six Australian nurses were attached to the RAAF hospital, assisting aeromedical evacuations. More than 12,000 casualties were flown out of Korea by the RAAF medical teams, often in difficult conditions.
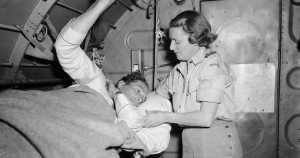
A RAAF nursing sister prepares a wounded patient for a medical evacuation from Korea to Japan. (AWM JK0184)
Like to copy this image? Please click here first
Working conditions
Australian medical personnel in Korea often worked in very primitive conditions, where access to running water, electricity and medical equipment was extremely difficult.
There were also psychological casualties. Medical personnel were sometimes called upon to help troops cope with the distress and trauma of what they faced.
Ill health after the war was a constant reminder to some men of their time in Korea.
(Extract from Out in the Cold, The Australian War Memorial's online exhibition on Korea)





